Clinical Guidelines (1st edition) 2023
The first three Clinical Guideline topics are now available to view and download.
The guidelines were developed with the support of Cochrane Repsonse (funded by NHS England) and the committment of our APPM Clinical Guidelines group. THANK YOU to all those whose committment and dedication enabled us to develop evidence-based clinical guidance for children and youg people with palliative care needs.
What are the Clinical guidelines?
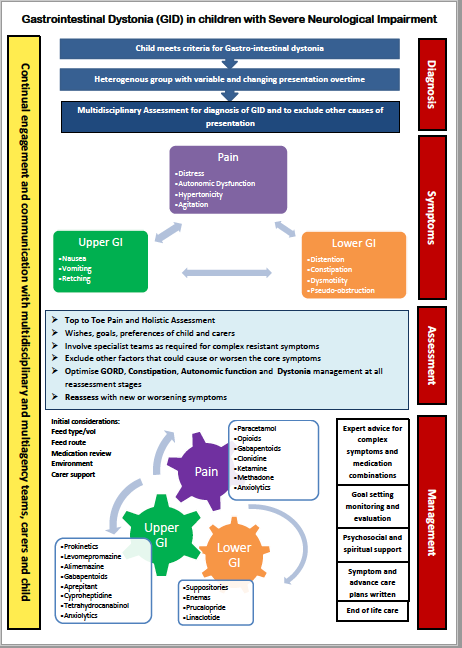
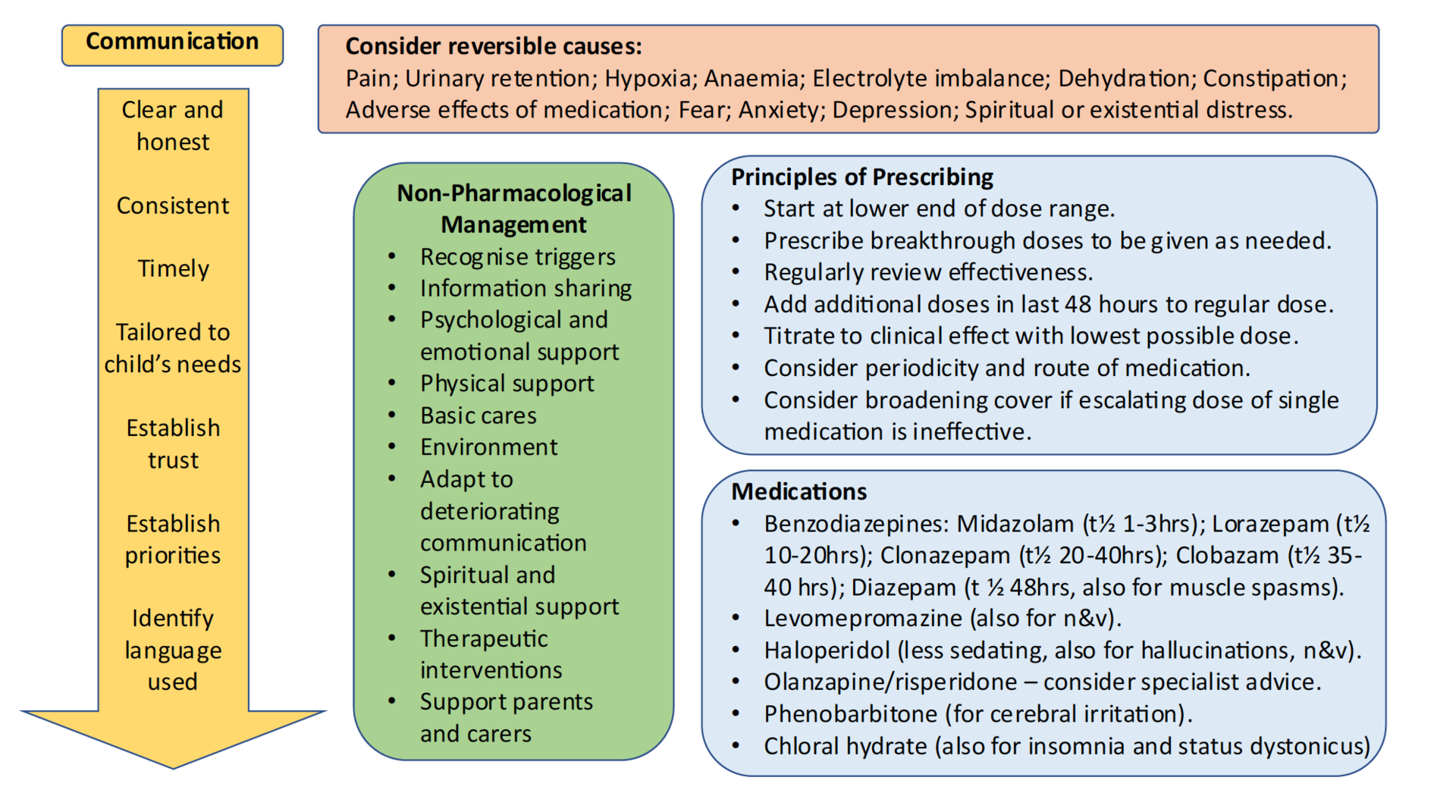
The APPM clinical guidelines seek to address symptoms, topic by topic, offering robust evidence-based, peer-reviewd clinical guidance to clinicians working with children and their families to support symptom management, palliatve and end of life care. The APPM members prioritised the symptoms in need of roubust guidance: Seizures, Agitation and GI Dystonia (initally called 'gut failure')
Clinical guidelines group:
The guideline group consisted of health professionals from medicine, nursing and pharmacy, parents and a previous service user.
The health care professionals came from primary, secondary and teritary services either working in paediatric palliative care or in aligned field where the professional was providing care to life limited children.
Thank you to our topic leads, the core topic group, wider guideline group, our reviewers and stakeholder
How the Clinical guidelines were developed:
Three symptoms were identified by the APPM membership as being key symptoms of concern that required prioritising for the development of evidence based guidance. A clinical guidelines group was formed and formation of the guidelines followed the RCPCH "Setting standards for the development of clinical guidelines in paediatric and child health. The details of the process are described in each topics methadology report and explaination for decision making is outlined in the Evidence to Decision tables for each topic (which provides evidence ratings of 'certainty' or 'robustness' of the gudiance given). The results of each topics systematic review, supported by Cochrane Response, their process is outlined here.
Feedback on Clinical Guidelines
We welcome your feedback on the three Clinical Guidelines that have been produced so far. Your opinion is very valuable to help with any improvement in these and future Clinical Guidelines.
Join our next Clinical Guidelines Group
We are planning our next two topics to start in in 2023: Pain and Dystonia. Please get in touch if you would like to be involved.
Evidence for
Information and resources to support revalidation and appraisal for doctors working in children's palliative care.
Evidence for
The Combined Curriculum in Paediatric Palliative Medicine aims to inform the training and assessment of all doctors who encounter dying children or those with life-limiting conditions.